Causes, Symptoms, and Treatments for Frozen Shoulders
Frozen shoulder, also known as adhesive capsulitis, is characterized by stiffness and pain in the shoulder joint. Signs and symptoms usually appear gradually and then worsen. Symptoms improve over time, usually within 1 to 3 years.
The need to keep a shoulder immobile for an extended amount of time increases the danger of acquiring a frozen shoulder. It could occur following surgery or a broken arm.
Range-of-motion exercises are used to treat frozen shoulders. Corticosteroids and numbing medicines are sometimes injected into the joint as treatment. Arthroscopy is occasionally required to release the joint capsule so that it can move more freely.
Frozen shoulder rarely recurs in the same shoulder. However, some people can get it on the other shoulder within five years.
What Is a Frozen Shoulder?
Frozen shoulder is a disorder that affects the joint of your shoulder. It is typically characterized by pain and stiffness that develops gradually, worsens, and then resolves. It can take anything between a year and three years.
The ball-and-socket joint in your shoulder is made up of three bones. Your upper arm (humerus), shoulder blade (scapula), and collarbone are all affected (clavicle). Tissue surrounds your shoulder joint and holds everything together. It is known as the shoulder capsule.
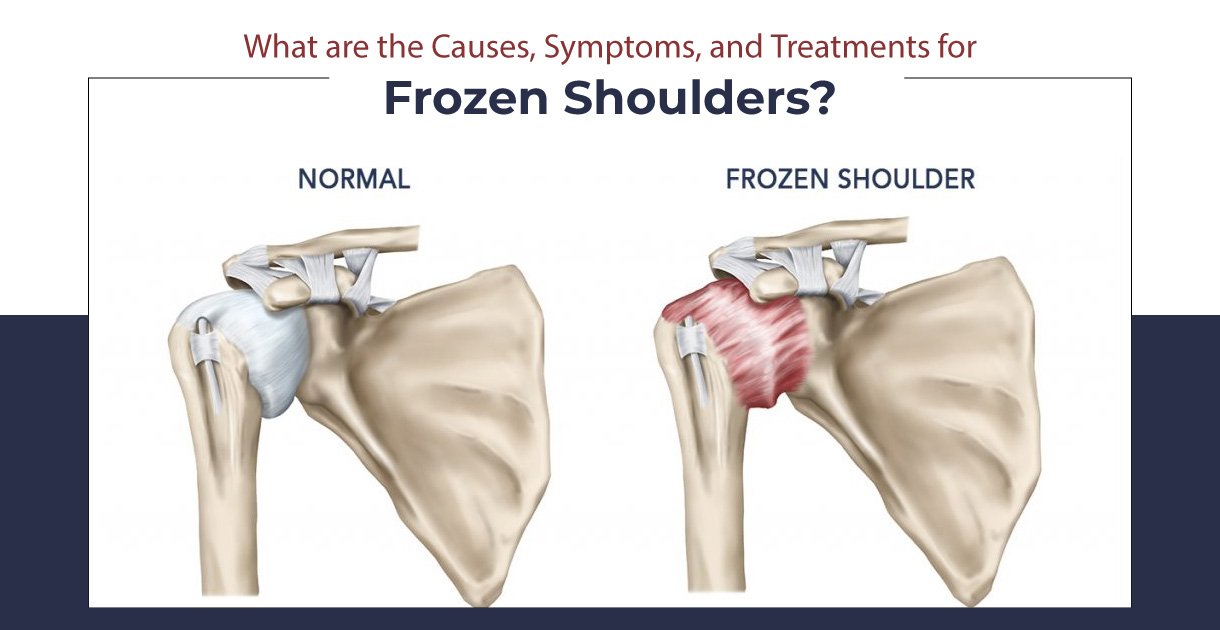
When you have a frozen shoulder, the capsule becomes so thick and tight that it is difficult to move. Scar tissue forms in the joint, and there is less synovial fluid to keep it lubricated. These things further restrict movement.
How Does Frozen Shoulder Occur?
Think of an accordion. The accordion has many folds when it is shrunk. Similarly, the connective tissue on the underside of the joint folds up when the shoulder joint is at your side.
A frozen shoulder’s folds stick together and do not easily unfold to allow a full range of motion. It produces significant pain and restricts shoulder joint movement.
Symptoms
Frozen shoulder usually develops in three stages.
Stage of freezing
Any shoulder movement generates pain, and the shoulder’s range of motion is restricted. This stage lasts between 2 and 9 months.
The stage is frozen. During this period, the pain may lessen. However, the shoulder stiffens. It becomes more difficult to use. This stage lasts between 4 and 12 months.
Stage of thawing The shoulder’s mobility begins to improve. This stage lasts between 5 and 24 months.
Some people’s pain worsens at night, affecting their sleep.
Causes
A connective tissue capsule surrounds the shoulder joint. Frozen shoulder occurs when the capsule around the shoulder joint swells and tightens, preventing movement.
It is unknown why this occurs in some persons. However, it is more likely to occur after holding a shoulder immobile for an extended period, such as after surgery or an arm fracture.
Risk factors
Certain things may raise your chances of getting frozen shoulder.
Age and sex
Frozen shoulder is more common in those over 40, especially women.
Immobility or reduced mobility
People who have had to maintain a shoulder somewhat motionless are more likely to acquire a frozen shoulder. Many factors can contribute to restricted movement, including:
- Rotator cuff strain
- Arm fracture
- Stroke
- Recovery from surgery
- Systemic illnesses
- Certain disorders appear to increase the risk of frozen shoulders.
Diabetes
- Thyroid hyperactivity (hyperthyroidism)
- Thyroid dysfunction (hypothyroidism)
- Cardiovascular illness
- Parkinson’s disease (PD)
Prevention
Not moving a shoulder while recovering from a shoulder injury, broken arm, or stroke is one of the most prevalent causes of a frozen shoulder. If you’ve suffered an injury that makes moving your shoulder difficult, talk to your doctor about exercises that can help you retain your capacity to move your shoulder joint.
How can a frozen shoulder be diagnosed?
Your doctor will perform the following tests to determine a frozen shoulder:
- Talk about your symptoms and go through your medical history.
- Examine your arms and shoulders physically:
- The doctor will move your shoulder in various directions to see whether there is any pain with mobility. This form of examination, in which your doctor moves your arm rather than you, is known as establishing your “passive range of motion.”
- The doctor will also examine your shoulder movement to determine your “active range of motion.”
- A comparison of the two forms of motion is made. Frozen shoulder patients have a reduced range of motion in both active and passive motion.
The best workouts for frozen shoulder
Pendulum sway
Perform this exercise first. Allow your shoulders to release tension. Stand up and lean forward gently, allowing the affected arm to dangle. Swing your arm in a one-foot-wide circle. Make ten spins in each direction once a day. Increase the stretch when you’re ready by swinging your arm with a light weight (three to five pounds).
Towel Stretch
With one hand, hold one end of a three-foot-long towel behind your back and the opposite end with the other. Keep the towel in a horizontal position. Stretch the injured arm by pulling your good arm upward. You can do an advanced exercise variant with the towel draped over your healthy shoulder. Hold the bottom of the towel with the affected arm and bring it toward the lower back with the unaffected arm. It should be done 10 to 20 times per day.
Walk your fingers
Approach the wall three-quarters of the way. Reach out and touch the wall at waist level with the fingertips of the affected arm. With your elbow slightly bent, carefully spider-like, walk your fingers up the wall until you can comfortably raise your arm. The effort should be made using your fingers rather than your shoulder muscles. Lower the arm slowly (with the help of the good arm if necessary) and repeat. Perform this exercise 10 to 20 times per day.
Final Words
Simple therapies, such as pain medications and shoulder exercises combined with a cortisone injection, are frequently sufficient to restore motion and function within a year or less. Even when left untreated, range of motion and shoulder usage improve independently, albeit at a slower rate. After around two years, patients are fully or nearly fully recovered.
If you are suffering from frozen shoulder challenges then consult top physiotherapist Dr. Niraj Patel at Om Physio Plus Nutrition.